Falls Screening and Prevention
If you have had a fall in the last 6 months or are concerned about being at risk of falling, talk to your doctor about your options to begin skilled care based on your specific needs.
Each year more than 1 out of every 4 adults age 65 years or older experience a fall. Although many falls do not result in serious injuries, about 20% of falls result in a serious injury such as a broken bone or head injury, with falls being the most common cause of traumatic brain injuries (1). Falls resulting in injury can make it challenging for an individual to care for oneself until they are fully healed and may need additional time to reach their previous level of strength and mobility to return to activities they enjoyed before their fall. If someone has had a fall resulting in no injuries, minor injuries (cuts and bruises) or hasn’t experienced a fall may develop a fear of falling resulting in more serious injuries. This fear of falling may restrict an individual from doing activities they normally enjoy or cause them to move less to avoid a fall. If someone is less active because of a fear of falling, they may become weak and actually increase their risk of a fall. This article will cover ways to screen for falls risk, factors that can influence risk of falls, and ways to lower fall risk.
Screen for Falls risk
Questionnaire
Here is a great checklist to assess your falls risk. Choose ‘Yes’ or ‘No’ to the following statements and tally up your score at the end (2).
| Answer | Statement | Why it matters | |
| Yes (2 points) | No (0 points) | I have fallen in the past year. | People who have fallen once are likely to fall again. |
| Yes (2 points) | No (0 points) | I use or have been advised to use a cane or walker to get around safely. | People who have been advised to use a cane or walker may already be more likely to fall. |
| Yes (1 point) | No (0 points) | Sometimes I feel unsteady when I am walking. | Unsteadiness or needing support while walking are signs of poor balance. |
| Yes (1 point) | No (0 points) | I steady myself by holding onto furniture when walking at home. | This is also a sign of poor balance. |
| Yes (1 point) | No (0 points) | I am worried about falling. | People who are worried about falling are more likely to fall. |
| Yes (1 point) | No (0 points) | I need to push with my hands to stand up from a chair. | This is a sign of weak leg muscles, a major reason for falling. |
| Yes (1 point) | No (0 points) | I have some trouble stepping up onto a curb. | This is also a sign of weak leg muscles. |
| Yes (1 point) | No (0 points) | I often have to rush to the toilet. | Rushing to the bathroom, especially at night, increases your chance of falling. |
| Yes (1 point) | No (0 points) | I have lost some feeling in my feet. | Numbness in your feet can cause stumbles and lead to falls. |
| Yes (1 point) | No (0 points) | I take medicine that sometimes makes me feel light headed or more tired than usual. | Side effects from medicines can sometimes increase your chance of falling. |
| Yes (1 point) | No (0 points) | I take medicine to help me sleep or improve my mood. | These medicines can sometimes increase your chance of falling. |
| Yes (1 point) | No (0 points) | I often feel sad or depressed | Symptoms of depression, such as not feeling well or feeling slowed down, are linked to falls. |
| Total:______________ | Add up the number of points for each “yes” answer. If you scored 4 points or more, you may be at risk for falling. | ||
| This checklist was developed by the Greater Los Angeles VA Geriatric Research Education Clinical Center and affiliates and is a validated fall risk self-assessment tool (Rubenstein et al. J Safety Res; 2011: 42(6)493-499). | |||
Five Time Sit to Stand Test
Equipment: standard chair (seat 17-18 inches from floor), stopwatch, assistant (optional)
Set up: Chair against wall to avoid sliding. Have an assistant or stable surface in front of the chair for additional safety.
Instructions: The goal of this test is to fully stand up and sit down five times as fast as you can without using your hands. The easiest way to make sure your hands aren’t being used is to cross your arms and rest your hands on top of your shoulders. Start the stopwatch when your assistant says ‘Go’ or you begin to start standing up. Stop the stopwatch when you sit down after your 5th repetition. Record your time. Do no use your hands to push off your knees or the armrest. Do not push the back of your legs against the chair to stand up. If you cannot stand up without using your arms, record 0 repetitions without using arms, and then record the time it takes to perform 5 repetitions while using your arms. If you cannot perform 5 repetitions then record the number of repetitions you can perform and proceed to the next test (3).
Scores: Use this table to find your age range and compare your number of repetitions to the number in the chart. If you scored less than the number in your age range you are at an increased risk of falls (4).
| Age | 60-64 | 65-69 | 70-74 | 75-79 | 80-84 | 85-89 | 90-94 |
| Female | 12 | 11 | 10 | 10 | 9 | 8 | 4 |
| Male | 14 | 12 | 12 | 11 | 10 | 8 | 7 |
Timed Up and GO
Equipment: Tape, standard chair, measuring tape, stopwatch, assistant (optional).
Instructions: The goal of this exam is to stand up, walk to the tape and then back to the chair and sit down as fast and as safely as possible. Measure 3 meters (9.8 feet) from the front of the chair and mark this spot with tape. You will begin seated in the chair. When the assistant says ‘Go’ or you begin to stand up, start the timer. Walk to the tape mark and turn around and walk back towards the chair, the assistant can stay close to you as you walk for additional safety. When you are seated in the chair the timer stops. Record your time. You may use any walking devices that you normally use (cane, walker, etc) to perform this test. It is recommended that you wear your usual footwear during this test for additional safety. (6)
Scores: You are at an increased risk of falls if this test took 14 seconds or longer to complete. (7)
Four Stage Balance Test
Equipment: Stop watch, assistant (optional)
Instructions: You may not use any assistive devices for this test. For safety, consider performing this exam in the corner of a room with your back facing the corner and a sturdy chair in front of you or in front of a counter with someone nearby to guard. This test consists of 4 stages with increasingly difficult positions to test your balance. The goal is to hold each position for 10 seconds. If you are able to hold a position for 10 seconds, move onto the next position, if you are unable to hold a position for 10 seconds stop the test.
Position 1: feet together (or as close together as you can get)
Position 2: semi tandem (feet together, one foot slightly in front of the other)
Position 3: tandem (one foot in front of the other. Heel to toe like on a tightrope)
Position 4: single leg (one leg off the ground) (8).

Scores: Unable to hold position 3 (tandem) for 10 seconds or position 4 (single leg stance) for 5 seconds is an increased risk of falls (8,9).
MCTSIB
Equipment: stop watch, pillow, assistant (optional)
Instructions: This previous article goes into detail about performing this test and what the results mean. This test has 4 different conditions that assess your ability to use the three senses for balance (discussed in more detail here). Finding what conditions are difficult for you is a good starting point to know what exercises to work on to improve your balance.
The screens provided above are meant to be a quick way to assess balance, strength, and walking speed to get a general idea of how you move. The more screens you do, the more information you have to assess your possible falls risk. Consult medical professionals if you’re concerned about your balance or mobility for additional testing, interpretation of your results and treatment specific for your needs.
Fall Risk Factors
Environment
Your home environment could contribute to falls. Making some changes to your environment like the suggestions listed below can make your home safer.
- Keep hallways, counters, tables etc free of clutter
- Remove throw rugs or secure them to the floor
- Secure power cords or move them from common walkways.
- Have good lighting in all rooms. Consider night lights or motion detecting lights for spaces such as hallways, bathrooms and bedrooms
- Have contrast between your floor and furniture. For example, having dark colored furniture and light colored floors will make it easier to see objects to avoid running into them or accidentally missing the furniture when sitting down.
- Keep commonly used objects in easy to reach places (drawers or lower shelves)
- Consider home modifications such as grab bars, shower chairs, bed railings, or raised commodes as needed
Changes to your home mentioned above can help reduce falls risk, but changing your home environment alone has not been shown to be as useful without additional interventions (10).
Health Factors
Everyone is different and has a different medical history. Here are a few health factors that can alter your risk of falls.
- Medications. Certain classes of medications can put you at an increased risk of falls. If you’re taking 4 or more medications you may also be at a higher risk of falls (11). Do not change your medications or stop taking them. Talk to your doctor to review your medications to make sure you’re taking medications that you need, at the right dose, and at the right time to optimize your health and safety.
- Neurologic function. Our nervous system helps us move our muscles, gives us the sense of touch, and helps communicate messages between our body and brain. Changes to the nervous system can alter how we move and make movement and balance challenging. Common conditions that affect the nervous system are Parkinson’s, MS, and stroke. Diabetes mellitus or neuropathy can alter the sensation in your feet, making it harder to feel the ground and stay balanced. Any condition involving the nervous system can affect people in different ways and will best benefit from treatment to fit their specific needs (12).
- Vision. Having poor vision can make it harder to see your environment and any obstacles. Vision is one of the three senses used in balance so it’s important to make sure your eyes are healthy and can clearly see your environment. Wearing glasses with multifocal or transition lenses can increase fall risk if you have trouble finding the edge between ground and surfaces such as stairs, curbs or chairs (13). Getting an eye exam if you have not had one in the last year to assess visual acuity, depth perception, and your current glasses prescription can assist in lowering your fall risk (1,13).
- Cardiovascular function. Certain changes in heart function or blood pressure can contribute to weakness, dizziness, and falls (14). Healthcare providers like your doctor or physical therapist can perform screens to assess your heartbeat and blood pressure and recommend further investigation if necessary. Here is a brochure from the CDC about changes in blood pressure when you change positions, a condition called postural hypotension, to learn about what it is and some ways to manage it (15).
Personal factors
- Alcohol. Consuming alcohol can alter your balance and coordination and can contribute to falls (12).
- Fear. A fear of falling may change the amount of activity you choose to do. A less active lifestyle can lead to decreased strength and balance, resulting in a higher risk of falls. If a fear of falling is keeping you from doing activities you enjoy, reach out to your doctor or a physical therapist for help. (12)
- Dizziness. Feeling dizzy can make it difficult to perform day to day activities and can also result in imbalance or feeling unsteady. If you’re experiencing dizziness, reach out to your doctor, an ENT specialist or a vestibular physical therapist in your area.
- Incontinence. Rushing to go to the bathroom has been shown to be associated with an increased risk of falls (16). Talk to your doctor or see a pelvic health physical therapist about managing feelings of urgency, frequent nighttime trips to the bathroom, or other issues of incontinence you may be experiencing.
Lowering falls risk
If you’re concerned about falling, reach out to a medical professional to assess and recommend treatments based on your specific needs. Listed below are ways to lower risk of falls based on information discussed above (12).
- Review medications with your doctor to ensure correct dosage and schedule
- Home safety evaluation and make changes to your home environment
- Eye exam every year and consider changing your glasses to a unifocal lens
- Feet exam to assess sensation
- Seeing medical professionals for any cardiac or neurological condition or any concerns you have about your health
- Seeking out care for symptoms of dizziness, incontinence, or urinary urgency
There are many programs designed to help with strengthening and balance. Some of these programs are: Otago, stepping on, STEADI, and tai chi for better balance (17). Look for programs in your area or ask a medical professional for recommendations of a program that will be best for you. Studies show that 50 hours of balance exercises over the course of 3-6 months is effective in lowering risk of a fall and can be conducted in an individual or group setting (18). It is important to make sure that these exercises are specific to what you need to improve on. Consulting a physical therapist to determine what strengthening and balance exercises are best for you, how to progress them, and additional information may be beneficial. Most active adults enjoy walking for exercise, and while this has many health benefits it has not been shown to influence risk of falls. If you enjoy walking, continue your regular routine but it is important to add exercises for balance in order to prevent falls (12). Listed below are some general strengthening and balance exercises that may help get you started.
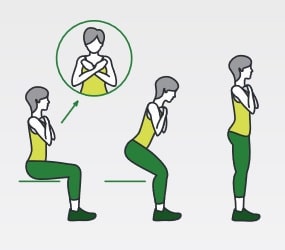
Sit to stand
Two screening tests for falls risk mentioned above looked at how well you can stand up and sit down without using your hands. If those screens were difficult for you, practicing this movement can help. If you have trouble standing up without using your hands, find a taller chair or stack cushions or pillows to raise the seat height so you can practice sit to stand without using your arms. Focus on slowly lowering yourself into the chair when sitting, and a strong push through the heels of your feet when standing up. A good challenge is a seat height where you can perform 8-10 repetitions of sit to stands with good form and a moderate amount of exertion. Perform 2 or 3 sets of this exercise. When you are able to perform 2-3 sets of 8-10 repetitions at a given height, progress the exercise by lowering the seat height or going from a firm chair surface to a soft chair surface or add additional weight to increase the challenge.
Step ups
Step ups are a great way to build strength with an everyday movement. If you have stairs in your home you can use the bottom step for this exercise. If you don’t have stairs, try a sturdy step stool next to your kitchen counter.
Calf raises
Facing a kitchen counter and both feet on the ground, push through your toes to lift your heels off the ground. Use the kitchen counter to hold for balance. Work up to 2-3 sets of 20 repetitions. When that is no longer challenging, progress to standing with one leg on the ground and performing heel raises.
Marching in place
Standing next to a counter to hold for balance, slowly march in place. The goal is to lift your knees up high and to move slowly. Try to do this without holding onto the counter but stay close in case you need to hold on. Progress to doing this without holding onto a surface, slowing leg movements, or ankle weights
Multidirectional walking (backward, sideways)
Face your kitchen counter so you can use both hands for balance. Continue to face your counter and side step along the length of your counter and back. Progress to side stepping without using your arms for balance, adding ankle weights or a resistance band around your knees for added resistance. You can also stand next to your counter in order to use one hand for balance and practice walking backwards. Focus on stepping with your toe first and weight shifting back onto your heel when you step backwards.
Standing balance
Perform standing balance along a counter for support, or in the corner of your house with the back of a chair in front of you. Look at your 4 stand balance test and mCTSIB results. What positions did you have trouble with? Working on the positions that were hard for you to perform will give you a better idea of where to start with some modifications to make you more successful. Once you can hold a position for 20 seconds, 3 times then you can increase the challenge. Here on some tips for modifying balance exercises:
- If feet together positions are difficult, place your feet slightly apart until you can hold a position for 20 seconds with mild difficulty and slowly move your feet closer together.
- If eyes closed positions are difficult, try eyes open with horizontal and vertical head turns and then progress to eyes closed with feet further apart. Progress by bringing your feet closer together.
- If foam positions are difficult, try a firm surface with feet close together or in semi tandem and then try foam with your feet wider apart and bring them closer as it gets easier
As always, to get the best outcomes and treatment based for you, talk to your doctor or physical therapist to get specialized exercises, treatment and instructions for your situation.
Sources:
(1) Center for Disease Control and Prevention. Important Facts about Falls. 10 Feb. 2017, www.cdc.gov/homeandrecreationalsafety/falls/adultfalls.html.
(2) Center for Disease Control and Prevention. Four Things You Can Stay Do to Prevent Falls: Independent. 2017, www.cdc.gov/steadi/pdf/STEADI-Brochure-StayIndependent-508.pdf.
(3) Shirley Ryan Ability Lab. Five Times Sit to Stand Test. 2013, www.sralab.org/rehabilitation-measures/five-times-sit-stand-test.
(4) Center for Disease Control and Prevention. Assessment 30 Second Chair Stand. 2017, www.cdc.gov/steadi/pdf/STEADI-Assessment-30Sec-508.pdf.
(5) Shirley Ryan Ability Lab. 30 Second Sit to Stand Test. 2013, www.sralab.org/rehabilitation-measures/30-second-sit-stand-test.
(6) Podsiadlo, D. and Richardson, S. (1991). “The timed “Up & Go”: a test of basic functional mobility for frail elderly persons.” J Am Geriatr Soc 39(2): 142-148. https://onlinelibrary.wiley.com/doi/abs/10.1111/j.1532-5415.1991.tb01616.x
(7) Physiopedia. “Timed Up and Go Test (TUG).” (2020) Physiopedia, www.physio-pedia.com/Timed_Up_and_Go_Test_(TUG).
(8) Center for Disease Control and Prevention. “Assessment Four Stage Balance Test.” Center For Disease Control and Prevention, 2017, www.cdc.gov/steadi/pdf/4-Stage_Balance_Test-print.pdf.
(9) Shirley Ryan Ability Lab. “Single Leg Stance or ‘One-Legged Stance Test.’” Shirley Ryan AbilityLab, 27 June 2013, www.sralab.org/rehabilitation-measures/single-leg-stance-or-one-legged-stance-test.
(10) Gillespie LD, Robertson MC, Gillespie WJ, et al. Interventions for preventing falls in older people living in the community. Cochrane Database Syst Rev. 2012;(9):CD007146. Excerpt: https://www.cochranelibrary.com/cdsr/doi/10.1002/14651858.CD007146.pub3/full
(11) Tinetti ME, Kumar C. The patient who falls: “It’s always a trade-off.” JAMA. 2010;303:258–266. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3740370/
(12) Avin KG, Hanke TA, Kirk-Sanchez N, McDonough CM, Shubert TE, Hardage J, Hartley G. Management of falls in community-dwelling older adults: Clinical Guidance Statement from the Academy of Geriatric Physical Therapy of the American Physical Therapy Association. Phys Ther. 2015;95:815–834. https://pubmed.ncbi.nlm.nih.gov/25573760/
(13) Lord SR, Smith ST, Menant JC. Vision and falls in older people: risk factors and intervention strategies. Clin Geriatr Med. 2010;26:569–581. https://pubmed.ncbi.nlm.nih.gov/20934611/
(14) Clinical Guideline 21 Falls: The Assessment and Prevention of Falls in Older People. London, United Kingdom: National Institute for Health and Clinical Excellence; 2013. Accessed June 22, 2017. https://www.nice.org.uk/guidance/cg161/resources/falls-in-older-people-assessing-risk-and-prevention-pdf-35109686728645.
(15) Center for Disease Control and Prevention . Postural Hypotension What It Is and What to Do About It , Center for Disease Control and Prevention , 2017. https://www.cdc.gov/steadi/pdf/STEADI-Brochure-Postural-Hypotension-508.pdf
(16) Soliman, Y., Meyer, R., & Baum, N. (2016). Falls in the Elderly Secondary to Urinary Symptoms. Reviews in urology, 18(1), 28–32. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4859925/
(17) Center for Disease Control and Prevention. “Older Adult Falls Programs.” Centers for Disease Control and Prevention, Centers for Disease Control and Prevention, 1 July 2015, www.cdc.gov/homeandrecreationalsafety/falls/programs.html.
(18) Sherrington C, Whitney JC, Lord SR, et al. Effective exercise for the prevention of falls: a systematic review and meta-analysis. J Am Geriatr Soc. 2008;56:2234–2243 https://www.laterlifetraining.co.uk/wp-content/uploads/2011/12/Sherrington_Ex_Int_Review_2008_JAGS.pdf